
Attention-deficit/hyperactivity disorder has been described as a risk factor for substance use disorder (SUD), possibly because of increased impulsivity and a deficit in the dopaminergic reward system, and SUD, especially the use of cannabis, has been described as a risk factor for PD. It is also possible that the association between ADHD and PD is mediated by other factors. Furthermore, prenatal factors, such as diabetes during pregnancy or neonatal complications, are also frequently reported as risk factors for both disorders. 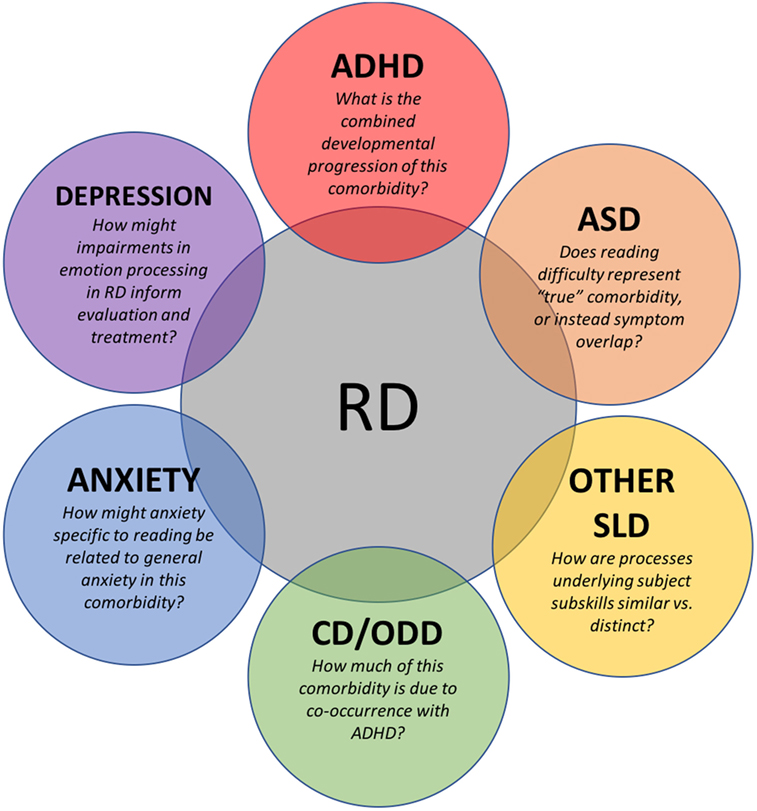 
The association between ADHD and subsequent psychosis could be explained considering many potential mechanisms, including shared genetic susceptibility or social environmental factors. The association remained high for the more restrictive diagnosis of schizophrenia. A recent metanalysis suggested an increased risk of psychotic disorder (PD), with a pooled relative effect of 4.74 (95% CI, 4.11–5.46) for patients with childhood ADHD. The research on neuropsychological processes has mainly revolved around executive function (EF) and theory of mind (ToM), emphasizing the presence of common etiological mechanisms and shared genetic risk factors. To date, little is known about mutual interactions between neurodevelopmental disorders, and the influence of psychosis on them. Age of onset constitutes another significant distinction between the two constructs. Conversely, positive symptoms, such as hallucinations and delusions, are defining features of schizophrenia but are not typically symptomatic of ASD. Catatonic features may also be present in both disorders. For example, difficulties with emotional reciprocity, or speech delay observed in ASD may be understood in terms of blunting of affect or alogia (poverty of speech) in schizophrenia, respectively. We should consider that ASD and schizophrenia are both characterized by atypical neuro-development of language and difficulties with social interaction and communication and ASD symptoms appear to overlap most significantly with negative symptoms of schizophrenia (see Table 1). 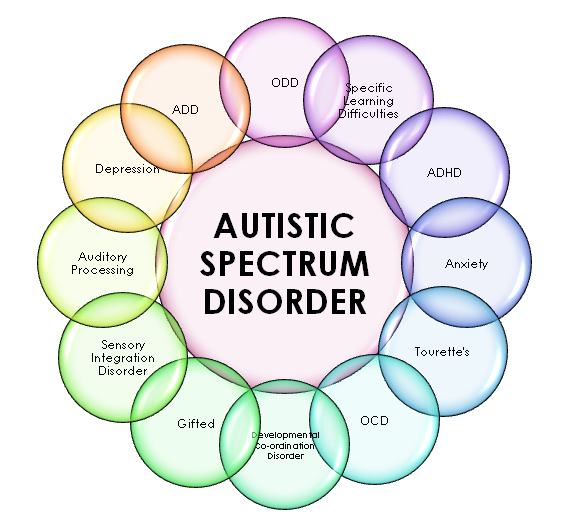
Moreover, psychotic disorders may further complicate these clinical pictures, resulting in diagnostic and therapeutic challenges for pediatric psychiatrists. Between 37–85% of Autism Spectrum Disorder (ASD) are estimated to present comorbid attention deficit hyperactivity disorder (ADHD) symptoms, with amplification of negative impact on quality of life. This work highlights the importance of a complete diagnostic assessment in patients with complex presentation, suggesting the possible overlap diagnosis of ADHD and Autism even in presence of psychotic-like symptoms.Ī high rate of multiple comorbidities in neurodevelopmental disorders is a common finding. Moreover, signs of attention and hyperactivity were consistent with ADHD diagnosis. Extensive clinic evaluation revealed a past medical and personal history of toe walking, weak social skills and stereotyped behavior observed and ADOS-2 Module 2 administration revealed severe Autism scores. Due to the worsening of clinical picture, several hospitalizations were necessary and pharmacological treatment with carbamazepine, risperidone and aripiprazole was carried out. At this time, auditory and visual hallucinations, as well as obsessive thoughts and attentional lability were also present and a diagnosis of “Early onset psychosis” was initially made. Here, we discuss the case of a nine-years-old boy presenting with an episode of abnormal sustained posture of the upper limbs, resembling dystonia, at the age of 3. Moreover, occurrence of psychosis can further complicate these complex clinical pictures. Autism Spectrum Disorder (ASD) and attention deficit hyperactivity disorder (ADHD) comorbidity is common in clinical practice and it seems to be related to shared etiological mechanisms and genetic susceptibility.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
